See It in Action
A real-time view of your MIPS performance.
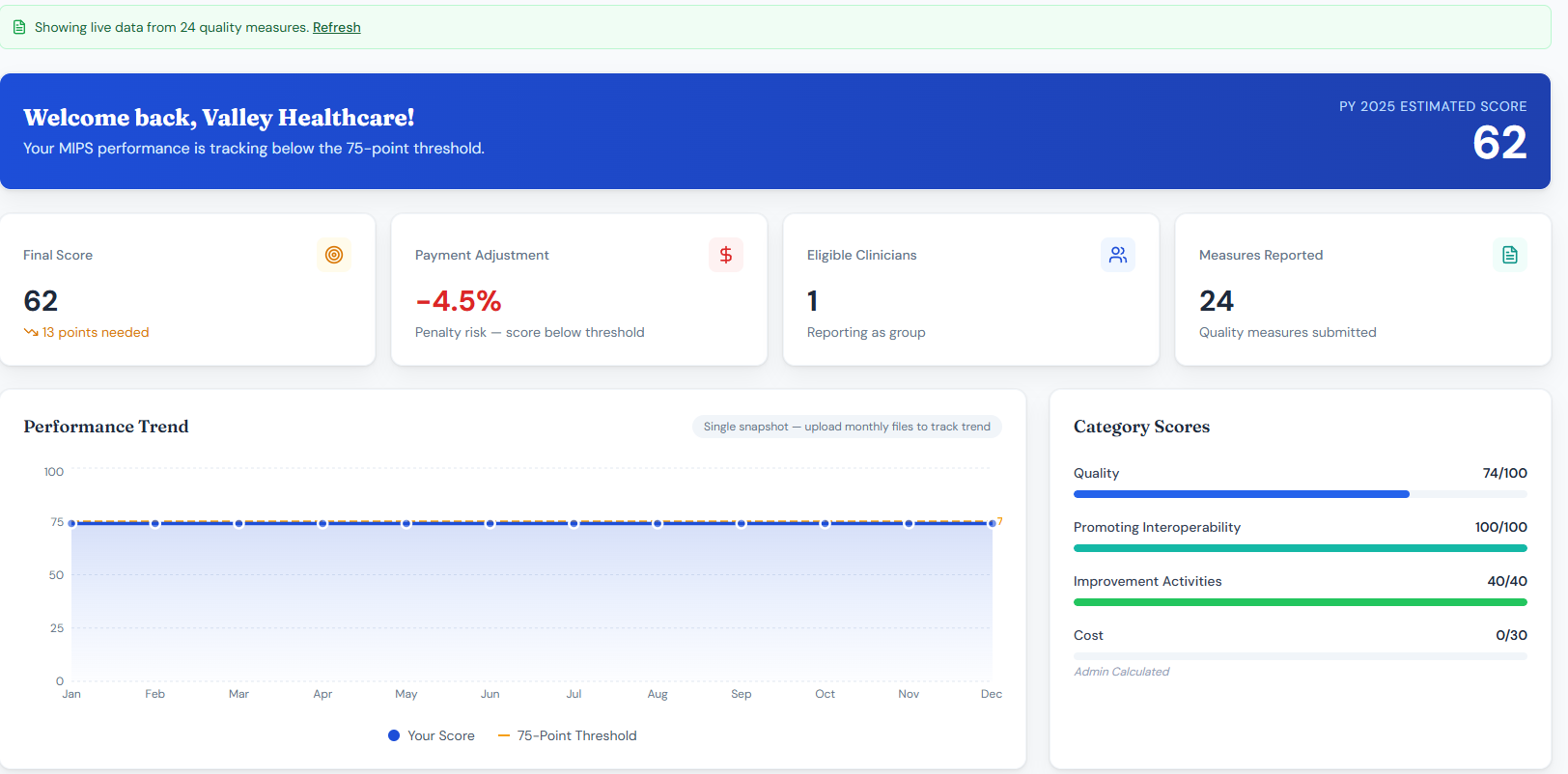
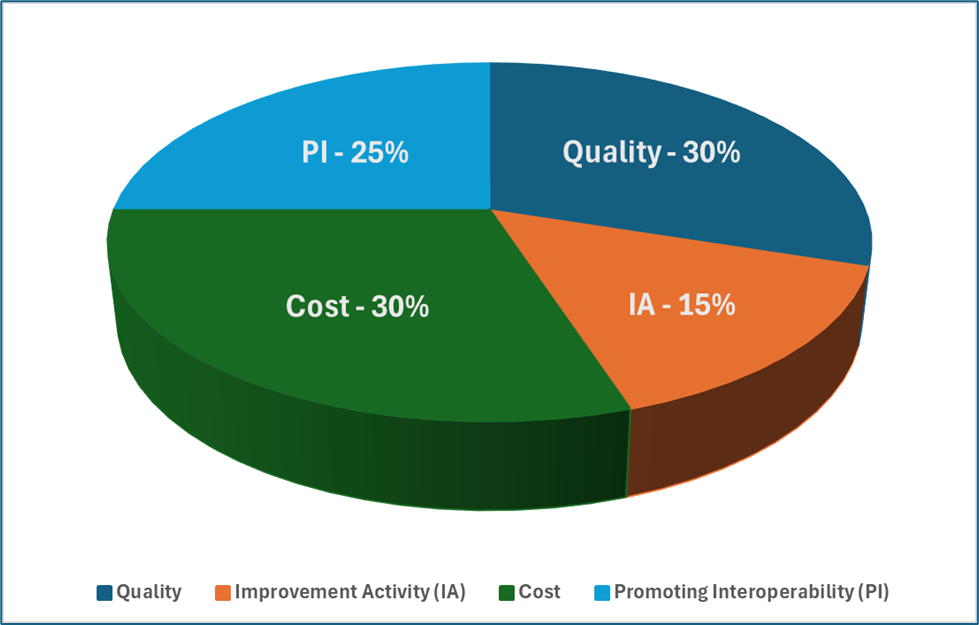

The EquityGuard Health™ QPP Solution helps healthcare practices track, optimize, and submit MIPS eCQM quality data — with real-time benchmark comparisons and a clear path to avoiding CMS payment penalties and qualify for quality-based incentives.
The EquityGuard Health™ QPP Solution is a cloud-based MIPS quality reporting platform designed specifically for healthcare practices participating in Medicare's Quality Payment Program (QPP).
Unlike generic dashboards, EquityGuard QPP integrates health equity data into your quality reporting — helping you understand not just how you're performing, but who may be underserved in your patient population.
The EquityGuard Health™ Portal delivers a comprehensive MIPS, MVP, and eCQM reporting solution for Providers and Clinicians' quality CMS data submissions, with confidence.
With real-time data imports and instant score calculation, your team has immediate visibility into performance rates, benchmark comparisons, and improvement opportunities.
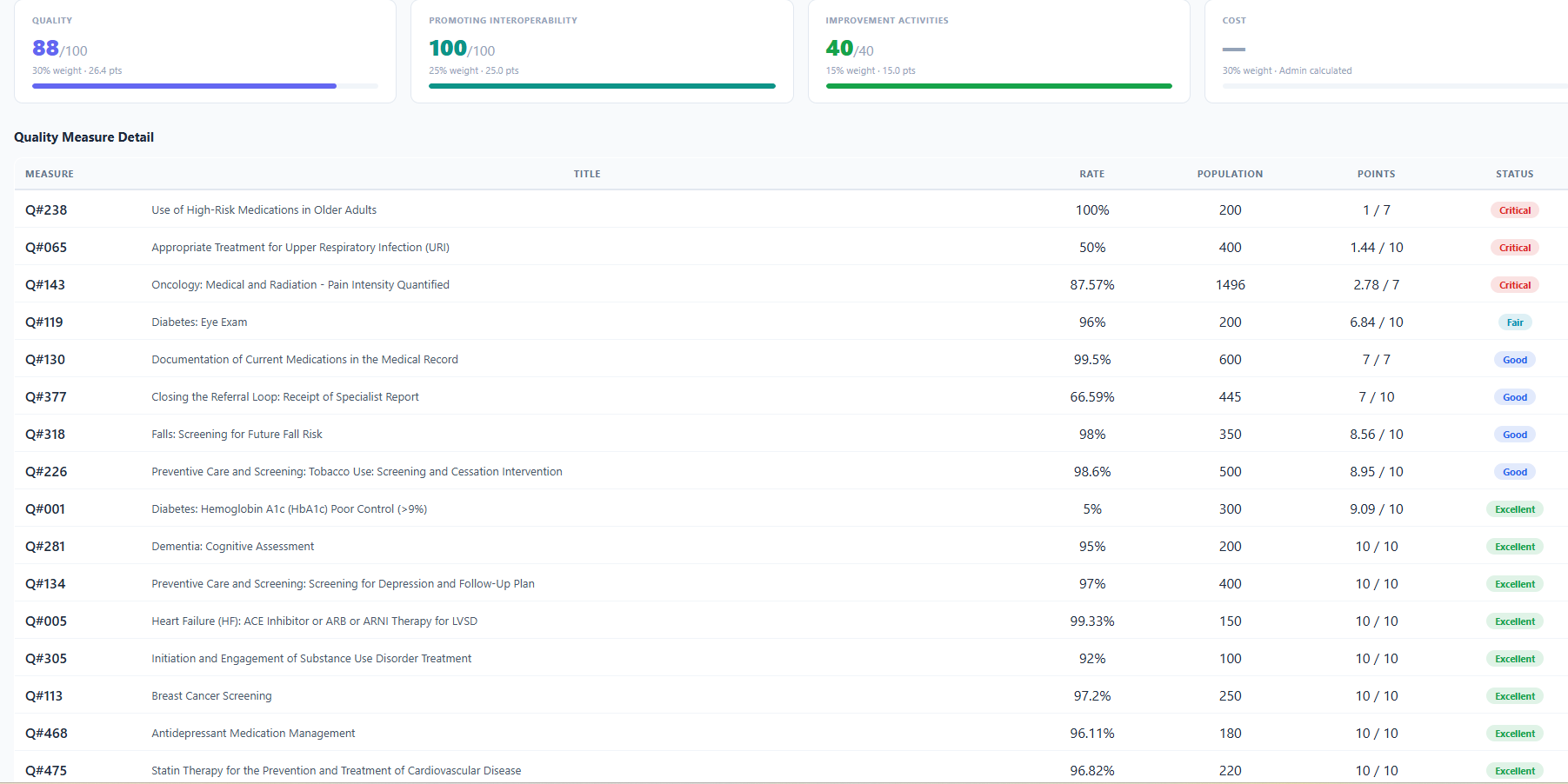
Full visibility across all active eCQMs, quality measures, and performance categories for the entire performance year.
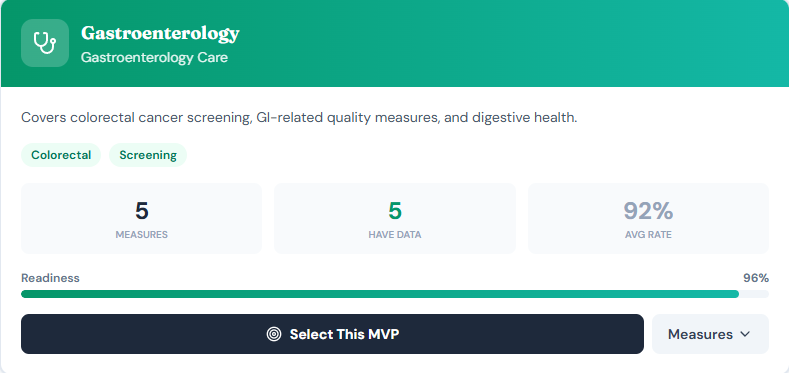
Our Pathway Analyzer compares Traditional MIPS vs. MVP side by side — choose the right path for your specialty.
Export a CMS-ready QPP files and branded performance report — streamlining your path from data to submission.
A real-time view of your MIPS performance.





Simple enough for small and medium-sized practices. Powerful enough for large healthcare organizations.
MIPS scores directly affect your Medicare payment adjustment for two years. A score below the 75-point threshold means a penalty on every Medicare claim you file — and that adds up fast for any practice with meaningful Medicare volume.
The EquityGuard Health™ QPP Solution shows you your exact score, which category is dragging you down, and what it would take to cross the 75-point threshold before the March 31 reporting deadline.
The latest from CMS on MIPS, MVP, value-based care, and quality reporting deadlines.
News and policy updates sourced from CMS.gov, qpp.cms.gov, and the Federal Register. Visit qpp.cms.gov for the most current information. Content is for informational purposes only.
The EquityGuard Health™ solution helps you determine and improve your overall Quality Score.
Powered by EHR Management LLC · EquityGuard Health™ Portal · Built on AWS